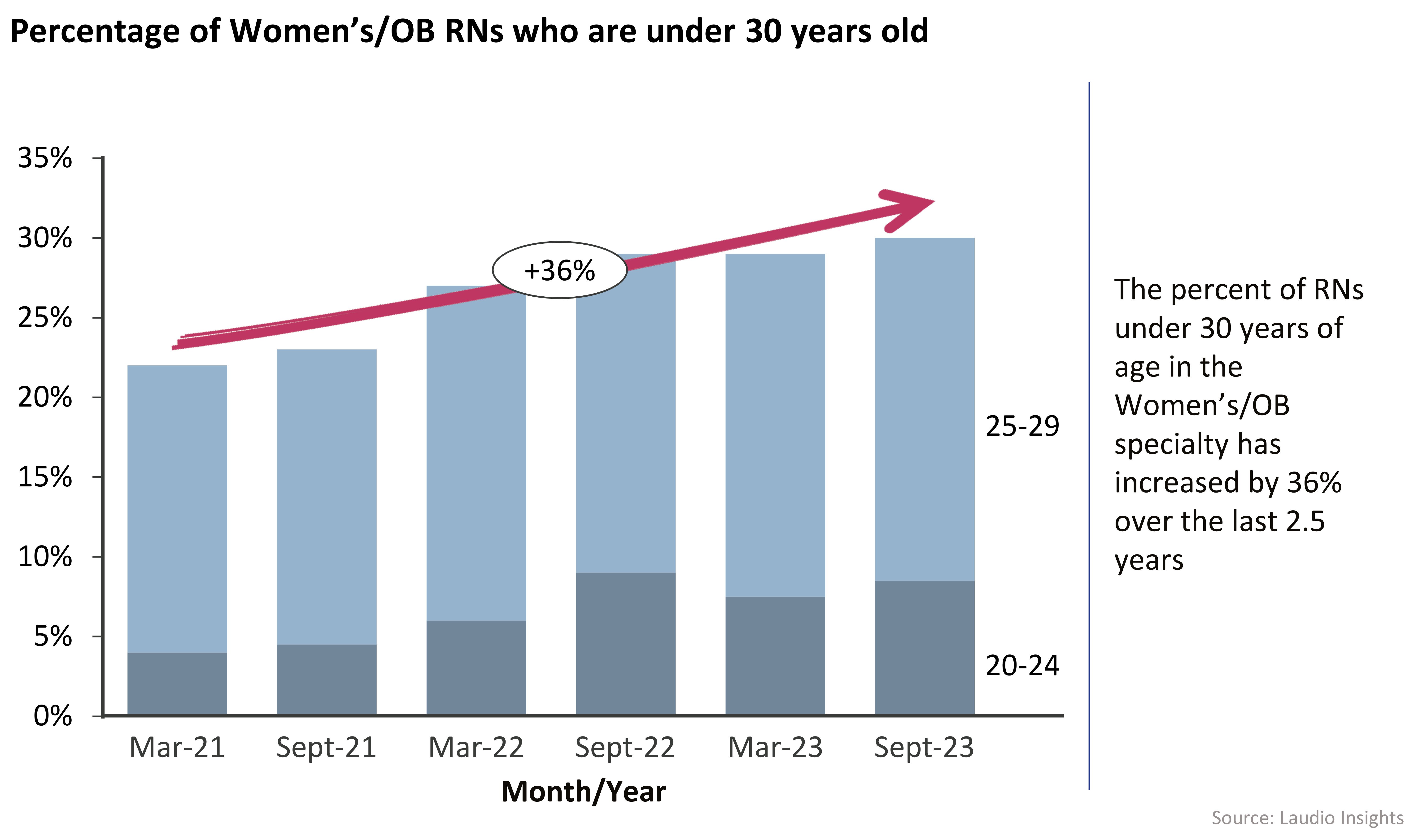
What the data says
Within Women’s Health/OB, which includes Labor and Delivery, Postpartum Care, and Nursery departments (but not NICU), the percentage of RNs under the age of thirty has increased over the last two to three years. In early 2021, younger RNs accounted for 22% of the RN team in this area; today, they represent 30%.
As more RNs have left Women’s Health (either due to retirement or moving to another unit or organization), an unusually high number of RNs in their twenties have been hired to replace them. These are RNs who, as recently as five years ago (before the retirements of the “Great Resignation” and the current acute nursing shortage), would have spent more time working in Med Surg units before transitioning into a complex specialty like Women’s Health.
What it means
An accelerated shift to an unusually youthful nursing workforce in Women’s Health has three main implications for health systems:
- Experienced RNs will shoulder greater responsibilities.
- A younger workforce represents a decrease in caregiver experience level in this highly specialized nursing practice. Experienced RNs within the specialty quickly become more crucial and in higher demand to support their more junior team members. Leaders must recognize the impact of this increasingly younger nursing team on the workload of the experienced RN in this demanding clinical specialty.
- While many new RNs are younger, health systems are still experiencing transfers from other specialties (and even non-nursing careers). Even with these experienced transfers, the overall percentage of younger nurses is increasing; these implications apply only to the less experienced specialty RNs.
- While an increase in specialty-based nurse residency programs has made this change possible, residency programs alone don’t provide all of the support that early-tenure RNs need.
- Residency programs within the specialty, along with preceptor programs, allow RNs to enter at early stages of their careers, but don’t offer support months and years later when new questions and growth opportunities arise.
- Cultural norms will adjust more quickly than normal.
- A large change in the generational mix of a department means that the culture will also change quickly, creating an ever-evolving set of requirements for leadership teams.
Annabelle Braun, the CNO at MemorialCare Orange Coast Medical Center, recently shared how her organization is adapting to some of these changes:
“We have definitely been seeing this change [a move to younger RNs in Women’s Health] over the last 10 years. It used to be that every nurse needed to do one, two, or three years in a Med/Surg unit before moving to a specialty. The pandemic accelerated the move away from that model. New grads want to go straight into specialties…
We welcome the change. We’ve built new grad programs. We have 3-12 month programs based on specialty. We have partnerships with neighboring schools of nursing to bring new grads into these programs which run in cohorts throughout the year." 1
Annabelle Braun, the CNO at MemorialCare Orange Coast Medical Center
What the implications are for healthcare leaders
- There is a renewed impetus for leaders to redesign care teams in order to enable experienced RNs to have a greater sphere of influence on the practice of early-tenure RNs.
- Redesign care teams to expand the influence of experienced RNs within the clinical specialty on the increasing numbers of younger RNs with less specialty experience.
- Consider virtual nursing support where experienced RNs serve as a “phone a friend” resource to RNs newer to the specialty.
- Develop meaningful recognition for the experienced RNs as they provide support to the less experienced RNs.
- As one Women’s Director shared recently, leaders have a responsibility to support their experienced team members. Being a preceptor is exhausting; in units where a few experienced team members consistently act as preceptors for new grads is overwhelmingly fatiguing. Just like departments need to create a pipeline for new grads, there is also a need to develop an internal pipeline for team members who can be in charge and precept.
- Post-residency support, such as professional development programs, now requires as much consideration as residency programs.
- A Labor and Delivery manager shared, “For new hires, we assign a ‘Team Buddy’ who shares similar interests and have them do virtual coffee before they start; so by their first day, they know at least one person who is immediately available.”
- A formal question-based and goal-setting meeting between team member and their managers at critical intervals (often referred to as new hire check-ins), which extend up to the 12th month of tenure, are highly impactful ways of building retention and independence in addition to specialty residency programs.
- Formal development programs, such as clinical ladders, that are directly connected to practical skills, competencies, and responsibilities have been most successful with RNs.
- The use of these programs, which can become available shortly after the end of residency, provides a framework for support. They reinforce the use of mentors and continual learning (ideally focused on practical skills that can immediately be put to use), which help generate confidence, especially for RNs early in their careers who are learning both how to be independent as an RN and how to practice within their specialty. While Women’s Health/OB is a highly desirable specialty, it is a particularly complex one with many unique and stressful clinical situations.
- For RNs in Labor and Delivery, early, repeated, and specific learning on high-risk events is also critical to building confidence and independence. This can include training and simulations on procedures like reviewing fetal heart monitoring and supporting a physician with a shoulder dystocia maneuver.
- This latter event is a particularly complex and coordinated one that requires refined assessment skills acquired through experience; these can be stressful to new RNs in the absence of a strong support structure stretching beyond a residency program. RNs with less experience in the specialty who don’t have a support structure identified and in place may be at greater risk for turnover.
- Finally, communicating support for RNs, Nurse Assistants, and other team members who want to go back to school to earn an NP degree or midwife certificate can help to develop long-term retention. As one HR leader shared, “Overall retention rates with these team members are generally higher if they work as per diem employees with us during these moments of career growth and transition.”
- The generational mix change will bring new norms about staffing models, use of technology to communicate, and an insistence on inclusivity that will require innovation from the Women’s Health/OB managers.
- Staffing models: The oldest members of Generation Z completed their bachelor’s degrees in 2019; the youngest will in 2034. Almost all of them did some of their schooling virtually; all of them have seen a large shift in remote and hybrid working models at the very beginning of their careers. While remote work for RNs in clinical care is not expected, flexibility and control of their schedules are.
- Static staffing models need innovation to avoid burnout and maintain the engagement and viability of a shifting workforce. A number of related experiments are happening across the country, such as increasing the use of per diem staff to decrease the traditionally heavy expectations for overtime and on-call. This can help appeal to a younger nursing workforce that desires fewer work hours and more work-life compatibility.
- Even when the staffing model cannot be readily adjusted, improving the scheduling platform used can elevate the experience of frontline team members. Simple approval processes (such as those done by an assistant manager) that allow RNs to swap shifts amongst themselves also provide a level of much-appreciated autonomy.
- The use of technology to communicate: Gen Z expects to have any training, HR documents, and protocols/processes they need available in an easy-to-access online platform. They expect their leaders to share department news and updates daily, weekly, and synthesized monthly both in-person and remotely. They expect the use of platforms such as texting and WhatsApp to be used for staffing and scheduling communications.
- An insistence on inclusivity: Gen Z is particularly aware of the decision processes regarding how growth opportunities are made available to team members, such as who is invited to join a committee. Adding a standing agenda item on unit-level staff meetings to reinforce organizational Diversity, Equity, Inclusion, and Belonging (DEIB) shared governance messages and reminding team members of the process and requirements for specific growth opportunities is a simple way to underscore support for fairness and inclusivity without creating additional meetings.
- Staffing models: The oldest members of Generation Z completed their bachelor’s degrees in 2019; the youngest will in 2034. Almost all of them did some of their schooling virtually; all of them have seen a large shift in remote and hybrid working models at the very beginning of their careers. While remote work for RNs in clinical care is not expected, flexibility and control of their schedules are.
1
Disclosure: A MemorialCare affiliate has made an investment in Laudio. Any quotes or content attributed to MemorialCare or any of its staff do not constitute a product endorsement or testimonial.
Written by Tim Darling
President of Laudio Insights
Tim Darling is a co-founder and President, Laudio Insights. With over 20 years of experience in healthcare technology, Tim has a real passion for using data and analytics to serve the challenges facing healthcare organizations. Prior to Laudio, Tim was on the leadership team of a healthcare education analytics company and he spent seven years as a consultant at McKinsey & Company. He has an MBA from Carnegie Mellon and BS degrees in Mathematics and Computer Science from the University of Maryland, College Park.
